TECHNICAL INFORMATION
Prodigy Advance Plus Dexa- Bone densitometry is one of the most advanced bone densitometry technologies available. In one scan, without re-positioning the patient, both “AP Spine” and “Dual Femur” exams are obtained in a single acquisition.
It also provides “Lateral Vertebral Assessment” of lumbar and thoracic spine in one fast acquisition, and reports the type and severity of vertebral body deformities based on a patient’s height.
If there is an existing fracture of a vertebral body, the risk of subsequent fracture doubles. LVA can detect the fracture and improves prediction of future fractures.
ADDITIONAL APPLICATION:
The Total Body Composition software provides percentages and absolute values for lean and fat mass.
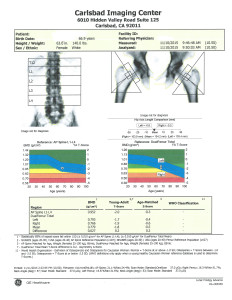
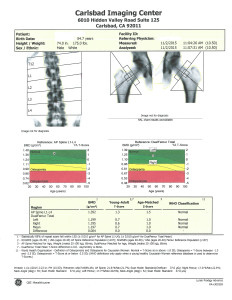
What is Fracture risk? Why is it important to me?
The bone densitometry test provides information about your own risk of bone fracture in the same way a cholesterol test indicates risk of a heart attack. A diagnosis of osteoporosis cannot predict a bone fracture, just as high cholesterol cannot predict a heart attack. Instead, it means that the risk of having a fracture is higher than that for normal bones. Your test results combined with other factors sum up your overall risk of fracture.
DEXA is most often used to diagnose osteoporosis, a condition that often affects women after menopause but may also be found in men and rarely in children. Osteoporosis involves a gradual loss of calcium, as well as structural changes, causing the bones to become thinner, more fragile and more likely to break.
DEXA is also effective in tracking the effects of treatment for osteoporosis and other conditions that cause bone loss.
The DEXA test can also assess an individual’s risk for developing fractures. The risk of fracture is affected by age, body weight, history of prior fracture, family history of osteoporotic fractures and life style issues such as cigarette smoking and excessive alcohol consumption. These factors are taken into consideration when deciding if a patient needs therapy.
Bone density testing is strongly recommended if you:
- Are a postmenopausal woman and not taking estrogen.
- Have a personal or maternal history of hip fracture or smoking.
- Are a postmenopausal woman who is tall (over 5 feet 7 inches) or thin (less than 125 pounds).
- Are a man with clinical conditions associated with bone loss.
- Use medications that are known to cause bone loss, including corticosteroids such as Prednisone, various anti-seizure medications such as Dilantin and certain barbiturates, or high-dose thyroid replacement drugs.
- Have type 1 (formerly called juvenile or insulin-dependent) diabetes, liver disease, kidney disease or a family history of osteoporosis.
- Have high bone turnover, which shows up in the form of excessive collagen in urine samples.
- Have a thyroid condition, such as hyperthyroidism.
- Have a parathyroid condition, such as hyperparathyroidism.
- Have experienced a fracture after only mild trauma.
- Have had x-ray evidence of vertebral fracture or other signs of osteoporosis.
The Lateral Vertebral Assessment (LVA), a low-dose x-ray examination of the spine to screen for vertebral fractures that is performed on the DEXA machine, may be recommended for older patients, especially if:
- They have lost more than an inch of height.
- Have unexplained back pain.
- If a DEXA scan gives borderline readings.
(Radiologyinfo.com)
5 Simple Steps to Good Bone Health
- Take daily calcium and Vitamin D
- Do regular weight-bearing exercise
- Avoid smoking and excessive alcohol
- Talk to your doctor about bone health
- Have a bone density test and take medication when appropriate
 Are you at risk for osteoporosis?
Are you at risk for osteoporosis?
By 2020 half of all Americans over 50 will have weak bones unless we make changes to our diet and lifestyle. People who have weak bones are at higher risk for fractures. Americans are living longer, and this means that our bones need to stay strong so we can be active and enjoy life. Strong bones begin in childhood. With good habits and medical attention when needed, we can have strong bones throughout our lives.
2004 Surgeon General’s Report on Bone Health and Osteoporosis
Frequently Asked Questions
Where can I get more information about bone measurements and osteoporosis?
The National Osteoporosis Foundation (NOF) is one of the leading sources of information about osteoporosis and bone measurements. The NOF recommends women have bone density test if you are:
- Over 65 years old
- Postmenopausal
- With a >1 risk factor
- With a fracture
- Considering osteoporosis therapy
- On prolonged hormone replacement therapy
The NOF recommends treatment if you have:
- A T-score < -1.5 with risk factors
- A T-score <-2.0 with no risk factors
- Had a fracture and are postmenopausal
Like other organs in the body, bones are constantly changing.
Throughout childhood and as young adults, bones grow in strength and in size. Around the age of 30, bones reach their peak strength and then naturally become weaker with age. Osteoporosis is a condition where bones become weak to the point of breaking.
Is the test safe?
Even though x-rays are used, the amount absorbed by the patient is only about 1/10th of that received from a chest x-ray. Other x-ray procedures have even higher x-ray doses. The x-ray dose from the bone densitometry test is comparable to the naturally occurring radiation you are exposed to in one week.
Caution: Even though the x-ray dose from the bone densitometry test is very low, please inform the operator if you are pregnant or might be pregnant before your test!
How does the densitometer work?
A bone densitometer measures bone mineral density (BMD). The amount of bone mineral relates directly to bone strength. The bone densitometer uses small amounts of x-ray to measure BMD and to produce images of the spine, hip, or even the whole body. The technical term for the method is “dual-energy x-ray absorptiometry”, or DXA. The spine and hip are measured because that is where most osteoporotic fractures occur.
What can I expect during my bone densitometry test?
The bone densitometer is a large, padded and comfortable examination table. You will be asked to lie on your back, remaining in your normal clothing in most cases. Belt buckles, metal or thick plastic buttons and metal jewelry will need to be removed from the region being examined. The operator will position your arms and legs for the test, which is painless and typically takes up to ten minutes. You just need to lie still and breathe normally.
How do I know if I have Osteoporosis?
Osteoporosis is often called the “silent disease”. There are rarely signs until a lot of bone has been lost. Visible symptoms may include a loss of height along with curvature of the upper back. Osteoporosis also can result in a crippling painful fracture, occurring most often in the hip, back, or wrist.
Important risk factors for osteoporosis include:
- Female
- Caucasian
- Advanced age
- History of bone fracture
- Small, thin frame
- Family history of osteoporosis
- Removal of the ovaries
- Early menopause
- A low calcium diet
- Lack of exercise
- Eating disorders
- Certain medicines (such as steroids or anticonvulsants)
- Alcohol and tobacco use
Contact the NOF at:
National Osteoporosis Foundation
251 18th St S #630
Arlington, VA 22202
(202)223-2226
www.nof.org

